Does Type of Diabetes affect Rejection, Infection, and Surgical Outcomes after Simultaneous Pancreas-Kidney Transplantation?
Eric Martinez1, Phuoc H. Pham2, Jesse F. Wang2, Lily N. Stalter2, Bridget M. Welch2, Glen Leverson2, Nicholas Marka2, Talal Al-Qaoud2, Didier Mandelbrot3, Sandesh Parajuli3, Hans W. Sollinger2, Dixon B. Kaufman2, Robert R. Redfield III2, Jon S. Odorico2.
1Transplantation, Baylor Annette C. and Harold C. Simmons Transplant Institute, Dallas, TX, United States; 2Department of Surgery - Transplantation, University of Wisconsin School of Medicine and Public Health, Madison, WI, United States; 3Department of Medicine - Nephrology, University of Wisconsin School of Medicine and Public Health, Madison, WI, United States
Introduction: Simultaneous pancreas kidney transplantation (SPKT) in Type 1 diabetes (T1D) patients with end stage renal disease (ESRD) has demonstrated acceptable outcomes, excellent pancreas allograft half-life, prolonged kidney graft survival (GS), preserved kidney graft ultrastructure and quality of life improvements. With an increase in SPKT performed in Type 2 diabetes (T2D) patients with ESRD, studies have found comparable results in SPKT for T1D and T2D regarding insulin resistance and β-cell function, kidney and pancreas GS, post-transplant glycemic control, and patient survival. An aspect insufficiently studied is the effect of diabetes mellitus (DM) type on allograft biopsy proven rejection (BPR), post-transplant de novo DSA (dnDSA), and post-transplant infectious and surgical complications. In this study, we comprehensively examine whether the type of DM, or related factors, impacts such outcomes.
Methods: Retrospective analysis of 345 primary SPKT recipients from 2006-2017 was undertaken with assessment of patient survival and GS, pancreas and kidney BPR, DSA development, readmissions, infections, and surgical complications (bleeding, pancreatic graft thromboses and surgical site complications). Minimum follow up was 1 year. DM type was determined by a holistic assessment with a grading system of patients’ age at DM onset, need for immediate insulin use, fasting C-peptide, family history of DM, and the presence of autoantibodies. Analyses were performed by Kaplan-Meier, log-rank test, and multivariable modeling.
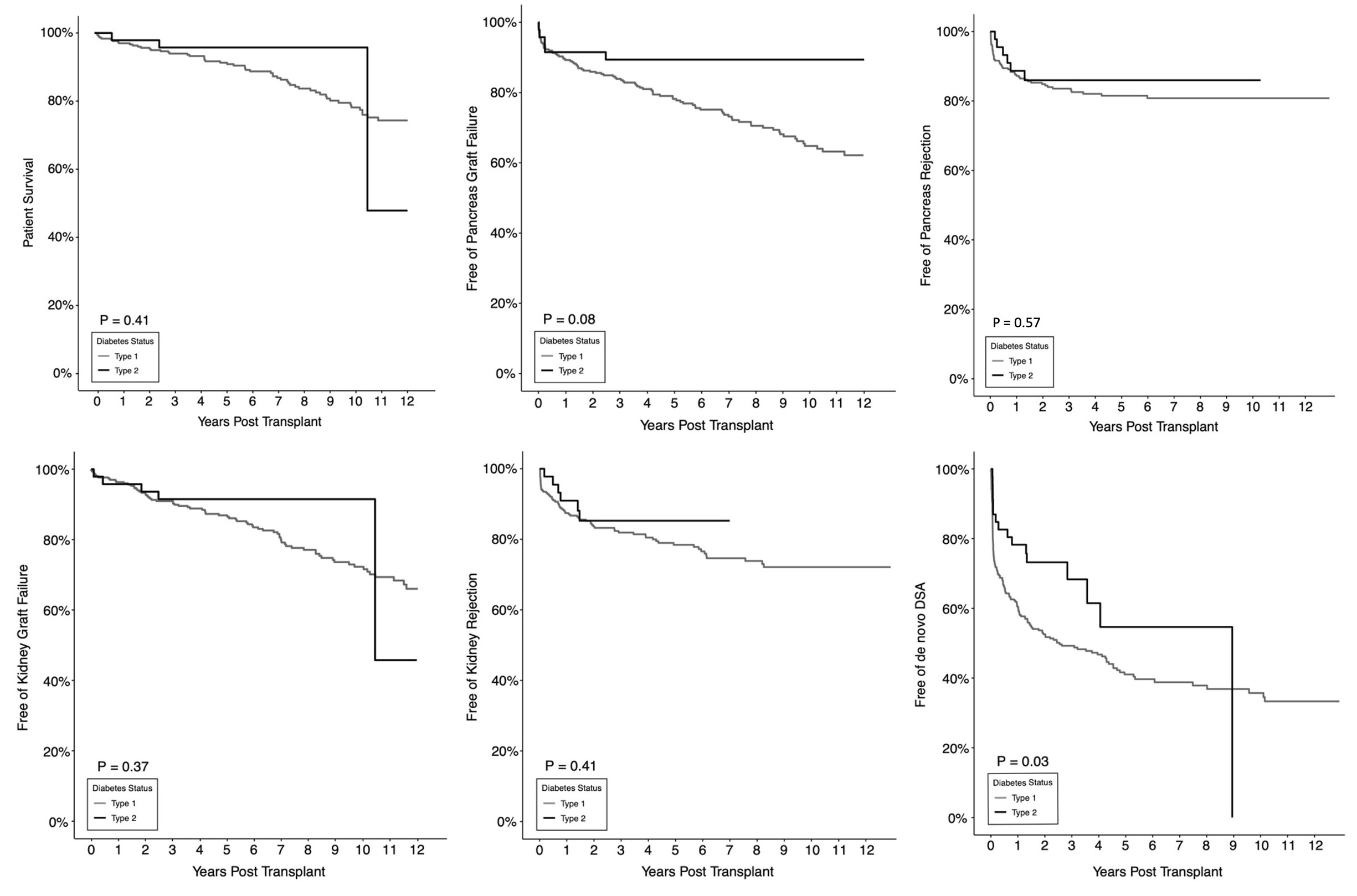
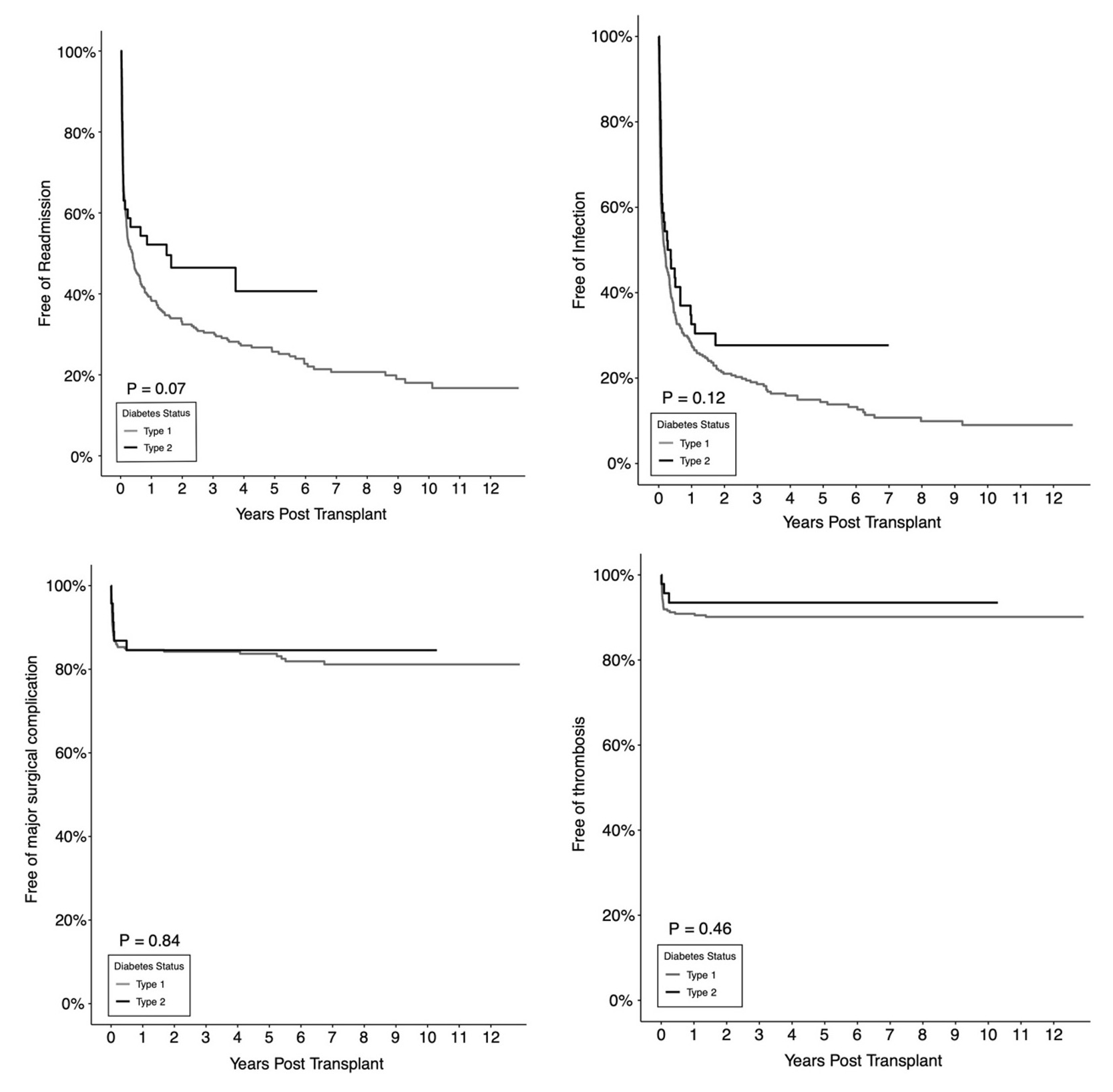
Results: Demographic variables were statistically significantly different (SSD) in T1D (n=298) vs T2D (n=47) recipients. There was no SD in outcome-free survival regarding patient or GS (pancreas or kidney) or BPR or other outcomes (Figure 1 and 2). The risk of BPR of either graft was not SD between T2D and T1D recipients (HRpancreas = 1.04, p = 0.93; HRkidney = 0.96; p = 0.93). T2D demonstrated a significantly higher dnDSA-free survival (p = 0.03) though there was no SD between the two types on multivariate analysis (HR = 0.70, p = 0.20). Interestingly, higher BMI was associated with lower risk of pancreas BPR (HR = 0.90, p = 0.01), de novo DSA (HR = 0.95, p = 0.02), UTI (HR = 0.95, p = 0.04) and thrombosis (HR = 0.88, p = 0.02). Compared to basiliximab, alemtuzumab was associated with lower risk of de novo DSA (HR = 0.38, p <0.01), while antithymocyte globulin was associated with a lower risk of kidney BPR (HR = 0.40, p = 0.04). There was no SD between T2D and T1D SPKT regarding readmissions (HR = 0.77, p = 0.25), infections (HR = 0.77, p = 0.18), major surgical complications (HR = 0.89, p = 0.79) or thromboses (HR = 0.92, p = 0.90).
Conclusions: In conclusion, BPR, infections, and surgical complications after SPKT are not significantly worse in T2D compared to T1D recipients supporting the position that T2D status should not restrict possible SPKT candidacy.
National Institute of Diabetes and Digestive and Kidney Diseases of the National Institutes of Health - Award Number T35DK062709.