Impact of successful Pancreas Transplantation on Patient Reported Hypoglycemia Outcomes
Ravinder Jeet Kaur1, Shafaq R. Rizvi1, Corey Reid1, Bradley K. Johnson2, Byron H. Smith2, Shelly K. McCrady-Spitzer1, Walter K. Kremers2, Patrick Dean3, Aleksandra Kukla4, Mark D. Stegall3, Yogish C. Kudva1.
1Division of Endocrinology, Diabetes, Metabolism, & Nutrition, Mayo Clinic, Rochester, MN, United States; 2Department of Biomedical Statistics and Informatics, Mayo Clinic, Rochester, MN, United States; 3Department of Surgery and Immunology, Mayo Clinic, Rochester, MN, United States; 4Department of Nephrology and Hypertension, Mayo Clinic, Rochester, MN, United States
Introduction: Poorly controlled Type 1 Diabetes (T1D) is associated with increased HbA1c, increased severe hypoglycemia, decreased hypoglycemia awareness and diabetic ketoacidosis. These comorbidities and decreased quality of life are indications for Pancreas Transplantation (PT). Limited data are available about patient reported outcomes (PROs) related to Hypoglycemia after PT. Therefore, we prospectively studied these PROs over a year after PT in patients with T1D.
Methods: Ten PT recipients were enrolled within a month after PT and completed 3 visits (V1, V2 & V3 at 4 weeks, 4 months and 1 year). At each visit, participants completed Hypoglycemia Fear Survey-II (HFS-II) and Clarke hypoglycemia unawareness survey. HFS-II is a 33-item questionnaire to measure behavior and worry subscales related to fear of hypoglycemia in patients with T1D. Behavior subscale (HFS-B) describes behaviors individual would engage in to avoid hypoglycemia or its consequences. Worry subscale (HFS-W) describes concerns related to hypoglycemia. Clarke questionnaire evaluates awareness of hypoglycemia based on responses to 8 questions, identifying awareness (A) or reduced awareness (R). The Clarke R score ranges from 0 to 7 with ≤ 2 indicating normal A, 3 as undetermined A and score ≥4 suggesting impaired awareness of hypoglycemia (IAH). We analyzed insulin independent and partial graft function on insulin separately. Statistical analysis was done using a linear mixed effects model.
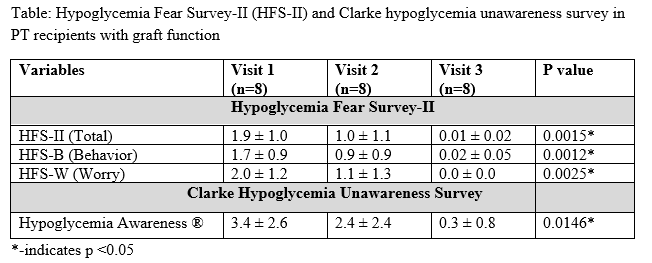
Results: Patients were 46.3 ± 14.3 years old, 9 F, duration of T1D 27.8 ± 15.8 years with 29.4 ± 18.3 days interval from PT. Laboratory results were HbA1c (%) 6.3, 5.4 and 5.4, fasting plasma glucose (mg/dL) 88.6, 104.8 and 91 and C-peptide (ng/ml) 4.6, 3.1 and 2.4 on V1, 2 & 3 respectively. In insulin independent participants (n=8), HFS-B showed almost every participant reported taking some behavioral measures over last 6 months to avoid hypoglycemia at V1. On V2, five participants took some behavioral measures and on V3 only one to avoid hypoglycemia (Table). HFS-W showed almost every participant had some concerns about low blood sugar at V1, five on V2 and none on V3. Two participants who had partial graft function around V2 engaged in behavior to avoid hypoglycemia on V1, 2 & 3, with a subsequent decreased behavioral engagement (p 0.1197) and concern to avoid hypoglycemia (p 0.1391) compared to V1.
Clarke scoring showed indeterminate awareness at V1, improved significantly (p 00.0146) and attained normal hypoglycemia awareness over the year on V2 and V3 respectively (Table). Two participants who had partial graft failure reported IAH on all 3 visits (V1: V2:V3=5.0: 4.0: 4.0, p 0.5000).
Conclusion: PT recipients reported reduced Fear of hypoglycemia and improved hypoglycemia awareness over a period of 1 year, even in patients with partial graft function. More studies would enable better assessment of these PROs and improve the field.